Urban Jaw Pain? Boston’s Dentist Deploys Botox TMJ Fix That Delivers SO Fast
Ever jolted awake with a sharp tightness in your jaw? Or noticed frequent headaches tied to tension that won’t fade? Urban Jaw Pain? TMJ Rehab Revolution Started In Boston: Botox In Just 48 Hours You’re not alone—this growing concern is sparking conversations across the U.S., especially among busy professionals and patients stress-tested by modern life. In Boston, a forward-thinking dentist practice has responded with a breakthrough approach: using Botox to target TMJ-related discomfort with remarkable speed and measurable results. This method is turning heads—not just for speed, but for how it fits into a world that values quick, non-invasive relief without long recovery times.
Recent digital trends show rising awareness around TMJ disorders, particularly in densely populated urban areas where stress, posture strain, and grinding habits fuel dysfunction. Boston’s dental community is stepping up, integrating neuromodulators like Botox into routine care as a fast-acting solution for urban-dwelling patients seeking immediate comfort. TMJ Rehab Revolution Started In Boston: Botox In Just 48 Hours This shift reflects a broader cultural move toward proactive, low-disruption healthcare tailored to fast-paced lifestyles.
How Botox Fights Urban Jaw Pain: The Science Behind the Fix
TMJ—the temporomandibular joint—is the hinge connection between your jaw and skull. When it becomes inflamed or misaligned, it triggers urban jaw pain: clicking sounds, limited movement, chronic discomfort, and even headaches. Traditional treatments range from splints and physical therapy to medication—but these often take weeks to ease symptoms.
Botox, a neuromodulator, works by calming overactive jaw muscles that contribute to tension. TMJ Suffering? This Boston Brand's Botox Breakthrough Outperforms The Rest TMJ Rehab Revolution Started In Boston: Botox In Just 48 Hours By inserting precision injections into specific facial muscles, dentists can reduce muscle hyperactivity, relieve pressure, and restore normal joint function—often within days. The Boston dentist team reports patients experiencing noticeable improvement in 48 to 72 hours, a dramatic contrast to slower conventional methods.
This targeted approach is backed by decades of research and refined through clinical practice, offering measurable relief without invasive surgery. The results are fast, tailored, and increasingly common in urban dental clinics aiming to meet rising patient demand for efficient care.
Common Questions About Botox for Urban Jaw Pain
How safe is Botox for TMJ relief? Botox used in TMJ treatment is FDA-approved and delivered by licensed dental providers trained in precise dosing and placement, ensuring safety and effectiveness.
How long does the relief last? Pause TMJ Pain Today×Boston's Hidden Secret For Instant Jaw Relief Most patients enjoy 3 to 6 months of significant improvement, after which treatments may be repeated based on individual needs.
Is Botox the only option? While Botox is effective, other approaches—like oral appliances, physical therapy, or stress-reduction strategies—may complement care. Your dentist can guide a personalized plan.
How much does treatment cost? Costs vary by location and treatment plan but typically range from $300 to $600 per session, factoring in clinical expertise and follow-up needs.
Will results come immediately? Unlike slow-acting medications, Botox reduces muscle tension within hours, with full effects emerging over 1 to 2 weeks.
Opportunities and Realistic Considerations
This emerging approach offers compelling advantages: speed, minimal downtime, and high patient satisfaction—values that resonate in fast-moving urban environments. However, it’s not a universal cure. Success depends on accurate diagnosis, consistent follow-up, and lifestyle factors like stress management and posture.
Many patients confuse Botox with cosmetic use, but in TMJ care, it serves strictly therapeutic purposes. Understanding this distinction builds trust and prevents confusion amid growing, sometimes conflicting, online claims.
For Boston residents and beyond, this botox-based TMJ solution represents a practical bridge between convenience and care—offering relief without disrupting modern life.
Debunking Myths About TMJ Botox Treatments
A common myth: Botox weakens jaw function over time. In reality, TMJ Botox temporarily relaxes specific muscles to reduce spasms and joint strain—supporting recovery, not damaging long-term function. Another misconception is it causes permanent numbness, but nerves are bypassed carefully in targeted injections.
Transparency and evidence guide current practice: patients are informed, monitored closely, and reminded this is part of a managed, medical-grade process—not a quick fix. This builds credibility and ensures informed decisions.
Who Might Benefit from This Botox-Based TMJ Approach?
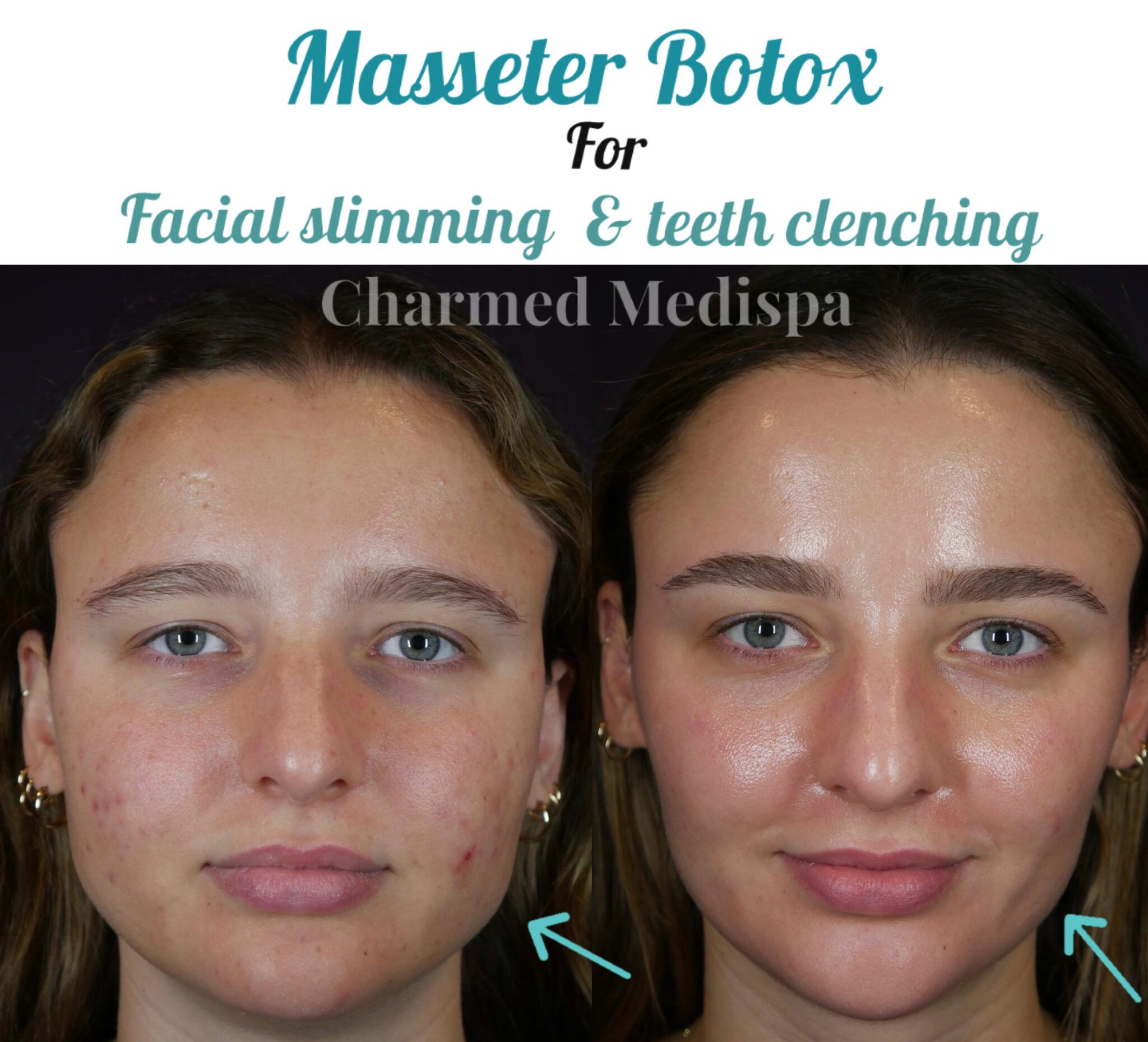
Urban Jaw Pain isn’t selective—anyone stressed by work, tech fatigue, or hidden bruxism (teeth grinding) can be affected. Young professionals, parents balancing tight schedules, and long-term city dwellers often report improved quality of life. Clinics emphasizing quick, tailored relief are seeing increased interest, particularly among patients seeking alternatives to prolonged physical therapy or invasive procedures.
This method is also gaining traction for travelers, remote workers, and anyone prioritizing discreet yet effective care—making it uniquely relevant to modern urban rhythms.
Looking Forward: Urban Care, Faster Relief
As urban living intensifies, so does demand for smart, time-conscious healthcare. Boston’s adoption of Botox for TMJ pain exemplifies this shift—a blend of innovation, patient-centered focus, and clinical reliability. While no single solution fits all, this approach highlights how modern dentistry is adapting to meet the pace and pain points of city life.
For anyone wrestling with urban jaw discomfort, exploring this non-invasive, rapid-response option could be a meaningful step toward comfort without compromise. Stay informed, ask your dentist about neuromodulator options, and consider how fast, science-backed care might align with your lifestyle.
The conversation continues—but clear, safe guidance is within reach.